Clinical implications of the neurosegmental level of injury in the treatment of hip dislocation and subluxation in children with spina bifida
- Authors: Baindurashvili A.G.1, Ivanov S.V.1, Kenis V.M.1
-
Affiliations:
- The Turner Scientific and Research Institute for Children’s Orthopedics
- Issue: Vol 4, No 4 (2016)
- Pages: 6-11
- Section: Articles
- Submitted: 28.12.2016
- Accepted: 10.01.2017
- Published: 14.12.2016
- URL: https://journals.eco-vector.com/turner/article/view/5889
- DOI: https://doi.org/10.17816/PTORS446-11
- ID: 5889
Cite item
Abstract
Background. Hip dislocation and subluxation are common in children with spina bifida.
Aim. To determine the influence of the neurosegmental level on surgical treatment of hip dislocation and subluxation in children with spina bifida.
Materials and methods. A total of 114 pediatric patients with spina bifida and hip dislocation and subluxation were treated at The Turner Scientific and Research Institute for Children’s Orthopedics (Saint Petersburg, Russia) from 2006 to 2015. The patients were divided into two groups according the Sharrard classification of neurosegmental lesions: a study group of 62 patients who underwent hip stabilization surgery and a control group of 52 patients who did not undergo hip stabilization procedures.
Results. For patients with a high neurosegmental level (thoracic and L1-L2), surgical treatment for hip dislocation and subluxation, which included most cases (72%), led to motor deterioration (retrospective study). Of 40 patients with a neurosegmental level of L3-L4 and L5-S1, motor level improved in 13 (32.5%) but deteriorated in 10 (36%) of 28 patients in the control group.
Conclusion. Determination of the neurosegmental level enables the prediction of motor level and reveals indication for surgical treatment.Full Text
Introduction
Spina bifida is caused by defective embryonic development of the nervous system and is accompanied by a complex set of clinical manifestations in the spine and spinal cord and in other areas, such as the musculoskeletal and genitourinary systems.
The orthopedic manifestations of spina bifida may be congenital in nature, and these form and progress during postnatal growth and development of the child. Congenital orthopedic manifestations of spina bifida include malformation of the spine, joint contractures, and deformation of the lower extremities caused by intrauterine effects of the neurological deficit on prenatal development. These are detected immediately after birth. Most orthopedic disorders have distinctive dynamics in the postnatal period. The development of the orthopedic effects of spina bifida is characterized by features unusual for the pathogenesis of other paralytic deformities with its main characteristics being muscular imbalance, trophic disturbances, aggravating impact of static and dynamic factors, and the absence of orthopedic prevention of deformities [1–3].
The hip joint defect in children with spina bifida is a frequent comorbidity and is commonly accompanied by the formation of hip subluxation and dislocation. According to various authors, 30%–50% of children with spina bifida develop subluxation or dislocation of the hip joint during the first 2–3 years of life [4]. Most scientists associate the formation of hip subluxation and dislocation with the nature of the primary lesion in the segmental apparatus of the spinal cord, specifically at the neurosegmental level [5].
Neurosegment refers to a specific portion of the spinal cord in a horizontal plane, giving rise to one pair of spinal nerves [6]. Both in foreign and Russian literature, there are several published reports on the effect of the neurosegmental level of involvement of spina bifida on the indications for treatment of orthopedic disorders [7–9].
The study objective was to determine the effects of the neurosegmental level of spina bifida on the outcomes of surgical treatment of hip subluxation and dislocation in children with spina bifida.
Materials and methods
A total of 114 pediatric patients with spina bifida and hip dislocation and subluxation were examined and treated at The Turner Scientific and Research Institute for Children’s Orthopedics (Saint Petersburg, Russia) between 2006 and 2015. All patients and/or their parents or guardians signed a voluntary informed consent to participate in the study and for surgery. To assess the hip joints, we used standard and functional X-ray projections. As an indicator determining the degree of gradation of disorders in the hip joint by radiography, we used the most common measurement, which is the migration index for the frontal plane. Hip subluxation was defined as a migration index value of more than 40%. Hip dislocation was characterized as a complete disconnection of the acetabular and femoral articular surfaces.
This study is a comparative analysis of the results of examination and treatment of patients divided into a study group and a control group. The study group consisted of 62 patients, who received surgical treatment to stabilize the hip joint, and the control group comprised 52 patients, who did undergo surgery for hip subluxation and dislocation.
To eliminate hip subluxation and dislocation, we performed reconstructive surgery, including interventions in the hip and pelvic components of the joint. Femoral bone osteotomy was performed in all cases of joint reconstruction by established procedures considering the initial parameters of the neck-shaft angle and the angle of antetorsion. The correction of changes in the pelvic joint component was performed based on the patient’s age, the acetabular index values, and the change in the value of the acetabulum rear edge angle.
During the examination, the neurosegmental level by Sharrard’s classification, based on the principle of the force evaluation (in points) of the major muscle groups of the lower extremities innervated by corresponding neurosegments, was determined [10] (Table 1).
Table 1. Classification of motor disorders by Sharrard’s neurosegmental level
Level | Muscular force | Neurosegmental level |
1 | Force of the plantar flexors of foot (4–5 points) | S2 |
2 | Force of the plantar flexors of foot (less than 3 points) Force of the tibia flexor (3 points) Force of the flexors and/or hip abductor muscles (2–3 points) | S1–L5 |
3 | Force of the hip flexors (4–5 points) Force of the tibia flexors (less than 3 points) Force of the extensors and hip abductor muscles (1–2 points) | L4–L3 |
4 | Absence of active extension of the knee joint Force of the hip flexors (adductor muscles) (less than 2 points) Raising the pelvis (3–4 points) | L2–L1 |
5 | Absence of muscle activity of the lower extremities Absence of the ability to raise the pelvis above the support surface in a horizontal position | Thoracic |
Two clinical subgroups were formed in the study and control groups of patients considering the involved neurosegmental level.
- Patients with lesions at high neurosegmental levels: thoracic and L1–L2 levels
- atients with lesions at low neurosegmental levels: L3–L4 and L5–S1 levels
Until 2009, the criterion for inclusion in the study group was the presence of hip subluxation or dislocation, regardless of the neurosegmental level of the lesion, and the criterion for inclusion in the control group was the presence of decompensated somatic pathology or refusal of parents for the surgical treatment (subgroup 1). After 2009, the criteria for inclusion in the study group were expanded to the presence of hip subluxation and dislocation and the involvement of neurosegmental levels L3–L4 and L5–S1, and the criteria for inclusion in the control group were contraindications for surgical treatment because of the presence of hip subluxation or dislocation and involvement of thoracic level and neurosegmental levels L1–L2, somatic pathology, or refusal of parents for the surgical treatment.
Fig. 1 shows the distribution of patients in the study and control groups.
In all the patients, the motor level was determined by a method proposed by the Medical University of Melbourne for children with consequences of spina bifida, which involves five levels of motor activity (Table 2).
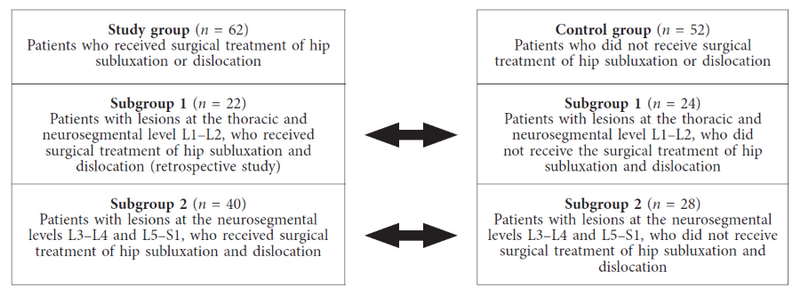
Fig. 1. The distribution of patients in the study and control groups
Table 2. Assessment of motor levels of patients with consequences of spina bifida, proposed by the Medical University of Melbourne
Functional capabilities of the patients | Motor level |
Ability to walk no worse than peers | 5 |
Walking with the use of orthoses of the ankle joint without additional support; using a wheelchair for long distance only. | 4 |
Walking within the home using orthoses and additional support; using a wheelchair both outside and inside the home. | 3 |
Walking during treatment at school for a limited time at home; using a wheelchair for moving. | 2 |
Absence of walking | 1 |
Motor level assessment was performed in patients before and after treatment.
Results and discussion
Based on the results of the examination and treatment, we performed a comparative assessment of the dynamics of the motor levels in patients with lesions at the thoracic level and neurosegmental level L1–L2 (subgroup 1) for the study and control groups. The results are shown in Fig. 2.
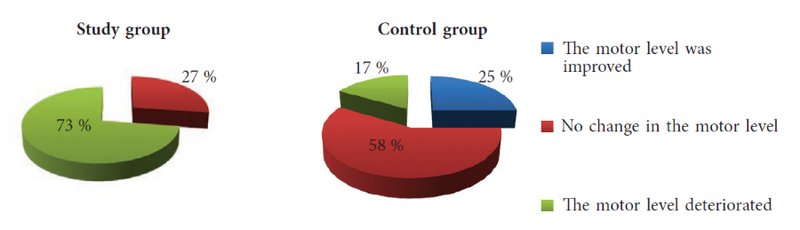
Fig. 2. Dynamics of the motor level in patients with thoracic level and neurosegmental level L1–L2 in the study and control groups
As seen from the data in Fig. 2, the motor level did not improve as a result of treatment in any of the pediatric patients in the study group, and in 16 of 22 (73%) patients, the motor level deteriorated. Our analysis of potential causes of this deterioration in the postoperative period showed that 16 of 22 patients had spontaneous fractures of the long bones of the lower extremities due to severe osteoporosis, which often occurs in patients with this condition.
We performed a comparative analysis of the incidence of fractures in patients with lesions at the thoracic level and neurosegmental levels L1–L2 in the study and control groups during the follow-up period. For patients in the study group, the number of fractures was significantly greater than that in the control group, with 14 of 16 (87%) patients experiencing more than two fractures. The patients with spina bifida are characterized by the appearance of fractures without any obvious trauma.
In the control group, the motor capabilities improved in six of 24 (25%) patients. In four of 24 patients, the motor capabilities deteriorated, and these deteriorations were associated with fractures that occurred during the rehabilitation treatment conducted. In the remaining 14 patients, the motor capabilities did not change. These patients had no contracture in the hip joints, which prevented them from sitting or lying down, and were able to move only by a wheelchair.
Thus, in patients with lesions at high neurosegmental levels (thoracic and L1–L2), the surgical treatment of hip subluxation and dislocation did not improve the motor level, and in the majority of patients (in our study in 16 of 22, i.e., 72%), their motor level deteriorated. The decrease in motor load in the postoperative period resulted in a decrease in bone density, the development of osteoporosis, and the formation of a “cascade” of fractures of the long bones, which inevitably led to the deterioration of motor abilities in the patient.
We also performed a comparative assessment of the dynamics of the motor level in patients with lesions at neurosegmental levels L3–L4 and L5–S1 in the study and control groups (subgroup 2). The results are shown in Fig. 3.
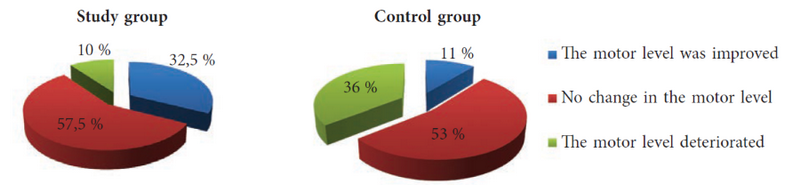
Fig. 3. The dynamics of the motor level in patients with lesions at neurosegmental levels L3–L4 and L5–S1 in the study and control groups
As seen in Fig. 3, surgical treatment of hip subluxation and dislocation in the study group improved the motor level in 13 of 40 (32.5%) patients. In 23 of 40 (57.5%) patients, the motor level remained at the preoperative level. At the time of the surgery, all patients had the highest possible motor level, and with timely surgical treatment, the achieved motor capabilities of the patient could be maintained. For the patients in the control group, the motor capabilities deteriorated in 10 of 28 (36%) cases.
Thus, surgical treatment of this patient population with hip subluxation and dislocation resulted in improvement of the motor level in 32.5% cases, whereas the absence of the surgical treatment resulted in motor level deterioration in 36.0% patients.
The results of these studies suggest that neurosegmental level of the lesion determines both the indications for surgical treatment of hip subluxation or dislocation and the motor level of the child.
Conclusions
- When planning surgical treatment of pediatric patients with spina bifida with hip subluxation and dislocation, the neurosegmental level of the lesion and the motor level of the child determine the indication of the treatment.
- The surgical treatment of hip subluxation and dislocation in pediatric patients with lesions at the thoracic and neurosegmental level L1–L2 is not indicated because it does not lead to an improvement in motor level.
- The surgical treatment of hip subluxations and dislocations in children with lesions at the neurosegmental levels L3–L4 and L5–S1 demonstrated an improvement of the motor level in 32.5% cases.
Information on funding and conflict of interest
This work was supported by the Turner Scientific and Research Institute for Children’s Orthopedics. The authors declare no obvious and potential conflicts of interest associated with the publication of this article.
About the authors
Alexei G. Baindurashvili
The Turner Scientific and Research Institute for Children’s Orthopedics
Author for correspondence.
Email: turner01@mail.ru
MD, PhD, professor, member of RAS, honored doctor of the Russian Federation, Director of The Turner Scientific and Research Institute for Children’s Orthopedics Russian Federation
Stanislav V. Ivanov
The Turner Scientific and Research Institute for Children’s Orthopedics
Email: turner01@mail.ru
MD, PhD, research associate of the department of foot pathology, neuroorthopedics and systemic diseases Russian Federation
Vladimir M. Kenis
The Turner Scientific and Research Institute for Children’s Orthopedics
Email: kenis@mail.ru
MD, PhD, professor, Deputy Director of Development and International Relations, head of the department of foot pathology, neuroorthopedics and systemic diseases Russian Federation
References
- Asher M, Olson J. Factors affecting the ambulatory status of patients with spina bifida cysticа. J Bone Joint Surg Am. 1983;65(3):350-6.
- Correll J, Gabler C. The effect of soft tissue release of the hips on walking in myelomeningocele. J Pediatr Orthop B. 2000;9(3):148-153. doi: 10.1097/01202412-200006000-00003.
- Feiwell E, Sakai D, Blatt A. The effect of hip reduction on function in patients with myelomeningocele. Potential gains and hazards of surgical treatment. J Bone Joint Surg Am. 1978;60(2):169-73.
- Erol B, Bezer M, Kucukdarmaz F, et al. Surgical management of hip instabilities in children with spina bifida. Acta Orthop Traumatol Turc. 2005;39(1):16-22.
- Баиндурашвили А.Г., Иванов С.В., Кенис В.М. Подвывих и вывих бедра у детей с последствиями спинномозговых грыж (обзор литературы) // Травматология и ортопедия России. – 2013. – № 4. – С. 97–102. [Baindurashvili AG, Ivanov SV, Kenis VM. Subluxation and dislocation of the hip in children with spina bifida (Review). Traumatology and Orthopedics of Russia. 2013;(4):97-192. (In Russ.)]
- Бадалян Л.О. Невропатология. – М.: Просвещение, 1987. – 316 с. [Badalyan LO. Nevropatologiya. Moscow: Prosvechenie; 1987. 316 p. (In Russ.)]
- Иванов С.В., Кенис В.М., Икоева Г.А., и др. Использование роботизированной двигательной реабилитации в комплексном лечении подвывиха и вывиха бедра у детей с последствиями спинномозговой грыжи // Ортопедия, травматология и восстановительная хирургия детского возраста. – 2014. – Т. II. – Вып. 4. – С. 32–35. [Ivanov SV, Kenis VM, Ikoeva GA, et al. The use of robotic rehabilitation in complex treatment of subluxation and dislocation of the hip in children with sequelae of spina bifida. Pediatric Traumatology, Orthopaedics and Reconstructive Surgery. 2014;2(4):32-5. (In Russ.)]
- Thomson JD, Segal LS. Orthopedic managment of spina bifida. Dev Disabill Res Rev. 2010;16(1):96-103. doi: 10.1002/ddrr.97.
- Yildirim T, Gursu S, Bayhan İA, et al. Surgical treatment of hip instability in patients with lower lumbar level myelomeningocele: Is muscle transfer required? Clin Orthop Relat Res. 2015;473(10):3254-60. doi: 10.1007/s11999-015-4316-8.
- Sharrard WJW. The segmental innervation of the lower limb muscles in man. Ann R Coll Surg Engl. 1964;35:106-22.
Supplementary files









