Guided Growth for Correction of Knee Flexion Contracture in Patients with Arthrogryposis: Preliminary Results
- Authors: Trofimova S.I.1, Buklaev D.S.1, Petrova E.V.1, Mulevanova S.A.1
-
Affiliations:
- The Turner Scientific and Research Institute for Children’s Orthopedics, Saint Petersburg
- Issue: Vol 4, No 4 (2016)
- Pages: 64-70
- Section: Articles
- Submitted: 10.01.2017
- Accepted: 10.01.2017
- Published: 14.12.2016
- URL: https://journals.eco-vector.com/turner/article/view/5897
- DOI: https://doi.org/10.17816/PTORS4464-70
- ID: 5897
Cite item
Abstract
Background. Knee flexion contractures frequently present in children with arthrogryposis and significantly alter kinematics of walking and reduce efficiency of ambulation or render it impossible. There are variety of surgical options for contracture correction, including entire soft-tissue release or its combination with Ilizarov ex-fix and supracondylar femoral osteotomy. Choosing of the most effective surgery is challenging because every method has limitations.
Aim. To evaluate the treatment outcomes of knee flexion deformity correction by guided growth in patients with arthrogryposis.
Materials and methods. A total of 12 patients (20 knee joints) with arthrogryposis who underwent anterior distal femoral hemiepiphysiodesis with 8 plates for knee flexion contracture correction were included in the study. The average age at surgery was 6.5 ± 0.5 (range, 4.3–9.6) years. Clinical and radiological methods were used with statistical analysis of the data.
Results. The mean preoperative knee flexion deformity angle was 48.5° ± 4.04° (range, 20°–80°). After distal femoral hemiepiphysiodesis, a reduction of knee flexion contracture was observed in 17 (85%) patients during a follow-up period of 18–36 months. The average correction was 20° ± 2.67° (range, 0°–40°) (p < 0.05). The residual deformity angle was 28.5° ± 6.03° (range, 0°–60°). Patients with contractures up to 50° demonstrated the most significant correction (by 90% compared with the initial value) (p < 0.05). This group included patients with severe flexion contractures, treated by serial casting, combined with an extension devise before surgery, which contributed to a significant reduction of the contracture.
Conclusion. Distal femoral hemiepiphysiodesis is an effective, safe, and reproducible surgical option for knee flexion contractures in patients with arthrogryposis. Combination with additional methods enables significantly reduction of knee flexion deformities from severe to moderate, thereby rendering treatment more effective with a shorter duration, which allows prompt improvement in ambulatory capacity.
Full Text
Introduction
Knee flexion contractures with arthrogryposis occur in 22%–67% of pediatric patients [1-3], considerably alter the kinematics of walking, and reduce the comfort of movement or make it impossible [4, 5]. Treatment with special exercises and staged plaster casts with orthotics should be started as soon as possible [6]. Surgical procedures for the treatment of rigid contractures include soft tissue release with or without an Ilizarov frame, extensor supracondylar osteotomy of the femur, and hemiepiphysiodesis of the anterior part of the distal femur growth zone. It is difficult to choose the most effective procedure as the release of soft-tissues often leads often to deformity relapses [2, 7]. Osteotomy cannot be used in growing children because of the high risk of bone remodeling [8]. Both Asirvatham (1993) and DelBello (1996) reported that the effect of supracondylar osteotomy was eliminated at the rate of 1° per month [9, 10]. Temporary hemiepiphysiodesis is safe and minimally invasive compared to other surgical procedures [2, 4, 11-13], but few reports on its use in the treatment of patients with knee flexion contractures with arthrogryposis have been published [4, 6, 12-14].
The aim of this study was to evaluate guided growth for correction of knee flexion contractures in patients with arthrogryposis.
Materials and methods
The study included 12 patients with arthrogryposis and knee flexion contractures (20 knee joints) who were treated by temporary hemiepiphysiodesis of the anterior part of the distal zone of femur growth with the use of figure-of-eight plates. The ratio of boys and girls was 2:1. Four patients had unilateral lesions, eight had bilateral lesions, and their average age at surgery was 6.5 ± 0.5 years (range, 4.3–9.6 years). The parents or guardians of these pediatric patients voluntarily gave signed informed consent for participation in the study and performance of surgery. Clinical evaluation included age at the time of the surgery, height, the extension deficit of the knee joint in degrees, and functional mobility according to the functional mobility scale (FMS version 2). Anteroposterior and lateral radiographs of the knee joints were obtained before and after surgery.
The surgical technique consisted of supraperiosteal parapatellar implantation of two figure-of-eight plates, each of which was fixed with two screws. Following this procedure, growth of the epiphyseal cartilage closer to the plate is decreased compared with that of the opposite side, which results in correction of the deformity. The ability to mount the plates was determined only by the size of the femoral condyles and not by the patient’s biological or bone age, i.e., the remaining function of the growth plate. The plates were placed 2–3 mm away from the medial and lateral edges of the patella, as contact with the patella can cause pain and limitation of motion of the knee joint. The screws were long enough to reach the opposite cortical bone layer but not pierce it. Immobilization was not required after surgery; the patients continued to use the ortheses while growth continued. Follow-up to evaluate contracture status and functional mobility of the patient was performed at 6-month intervals. The deformity correction rate was calculated in degrees per month. The plates were removed only after full correction of knee joint contracture.
Results were reported as arithmetic means ± standard error of the mean (SEM) and differences in mean values were tested with the parametric Student’s t-test. Statistical significance was determined by a table of critical values of the t-test depending on the sample size. The critical level of significance when testing the statistical hypotheses was taken to be equal to 95% (p ≤ 0.05). The data processing was performed using Excel 2010 and Statistica 6.0 software.
Results
Evaluation of the effectiveness of temporary blocking of the femoral growth zone for correction of knee flexion contracture was performed in 12 patients with arthrogryposis. The treatment period ranged from 18 to 36 months (average 22.7 ± 1.08 months). The average value of the knee extension deficit before surgery was 48.5° ± 4.04° (20°–80°), and patient height was 1.15 ± 0.04 meters (range 0.9–1.4 meters) (Table 1). The moderate contractures (20°–50º) were noted in 10 patients and severe contractures (≥50°) in ten. Before treatment, six patients did not walk because they could not maintain balance without support. One patient moved independently but for short distances only. The remaining five patients walked with accessory support.

Fig. 1. Patient S., 5 years of age, with arthrogryposis affecting the upper and lower extremities: a, flexion contracture of the left knee joint of 90º; b, lateral X-ray image of the knee joint prior to treatment; c the correction of the left knee contracture using a plaster cast and the distraction device; d, view of the knee joint (extension deficit of 40º) and f, its lateral X-ray image prior to hemiepiphysiodesis; e.g., 15º residual contracture of the knee joint 18 months after treatment initiation
Prior to surgery, conservative elimination of knee contracture was attempted in four patients using plaster casts and a distraction device (Fig. 1) [15]. Full correction not was achieved in any of them because of the development of pain in the knee joint, or signs of femoral condyle compression or tendency to tibia subluxation in X-ray images of the knee. However, with the use of additional methods of correction, the flexion contractures were reduced by 38.32º ± 4.6º (range 20º–50º), p < 0.05.
Table 1. Patient characteristics before and after knee surgery
The patient’s number | Age at the time of surgery, years, months | Deficiency of extension prior to the surgery, ° | Residual deformity, ° | Follow-up period, months | Rate of correction, degrees per month |
1 | 4,3 | 50 | 30 | 24 | 0,8 |
1 | 4,3 | 50 | 30 | 24 | 0,8 |
2 | 4,6 | 70 | 60 | 18 | 0,6 |
2 | 4,6 | 60 | 60 | 18 | 0 |
3 | 5,1 | 80 | 60 | 24 | 0,8 |
4 | 5,2 | 30 | 0 | 30 | 1,0 |
4 | 5,2 | 30 | 0 | 30 | 1,0 |
5 | 5,4 | 40 | 10 | 24 | 1,3 |
6 | 6,1 | 70 | 60 | 24 | 0,4 |
6 | 6,1 | 70 | 60 | 24 | 0,4 |
7 | 6,7 | 35 | 0 | 24 | 1,5 |
7 | 6,7 | 35 | 0 | 24 | 1,5 |
8 | 6,8 | 40 | 0 | 30 | 1,4 |
9 | 6,9 | 40 | 15 | 18 | 1,4 |
9 | 6,9 | 40 | 15 | 18 | 1,4 |
10 | 8,8 | 70 | 50 | 18 | 1,7 |
11 | 9,3 | 20 | 0 | 18 | 1,1 |
11 | 9,3 | 20 | 0 | 18 | 1,1 |
12 | 9,6 | 60 | 60 | 36 | 0 |
12 | 9,6 | 60 | 60 | 36 | 0 |
After hemiepiphysiodesis of the distal femur growth zone, decrease in knee flexion contracture was noted in 17 patients (85%). The amount of residual deformity was 28.5° ± 6.03° (range 0°–60°). The correction of the flexion contracture observed during follow-up period was 20° ± 2.67° (range 0°–40°), p < 0.05. Differences of effectiveness and the rate of deformity correction were found in patients with initial flexion contractures <50° and those with initial ≥50° (Table 2). In the first group (10 patients), the average deformity correction was 29° ± 2.1° (20°–40°), which was a change of 90.1% ± 5.2% (range 63%–100%). In the second group (10 patients), the flexion contracture decreased by an average of 11° ± 2.8° (0°–20°), which was a change of 47.4% ± 11.8% (range 0%–86%). The difference in degrees of flexion contracture correction in the two groups was statistically significant (Student’s t = 3.31, p < 0.05). Differences in correction in patients of different age were not significant.
Following treatment, functional mobility according to the FMS scale increased in eight patients. Three patients (4, 5, 8) who walked with the help of a supporting device before treatment were able walk independently within the premises, and four patients (1, 7, 9, 10) who did not walk before treatment were able to maintain balance and walk with support. One patient (11) who walked independently prior to treatment was able to walk faster and the walking distance increased from 50 to 500 meters. One complication, fixing screw migration, was noted, and the figure-of-eight plate was implanted in that patient again.
Table 2. Knee joint contracture in patients with an initial contracture of <50° and ≥50°
Group of patients | Contracture,° | Deficiency of extension prior to the surgery,° | Residual deformity,° | Amount of correction,° | |||
mean | range | mean | range | mean | range | ||
1 | < 50 | 33 ± 2.5 | (20–40) | 4 ± 2.1 | (0–15) | 29 ± 2.1 | (20–40) |
2 | >50 | 64 ± 3.1 | (50–80) | 53 ± 3.9 | (20–60) | 11 ± 2.8 | (0–20) |
Discussion
Most researchers agree that the use of manipulation during bone growth is reasonable, safe and effective. The short period of immobilization, minimal invasiveness compared with other techniques, a relatively simple surgical technique, and a low rate of complications are all advantages of this method [2, 4, 6, 11-14, 16].
In this patient series, temporary hemiepiphysiodesis of the anterior part of the distal zone of femur growth reduced the amount of flexion contracture of the knee joint, or eliminated it completely, thereby improving the functional mobility of patients with arthrogryposis. Decrease in the flexion contracture occurred in 85% of the patients, and the average correction was 20° ± 2.67° (range 0°–40°). Full extension of the knee joint was achieved in one–third of the patients, but only reducing the extension deficit of the knee joint, significantly improved the functional mobility of four patients (Fig. 2). In all eight, the correction occurred within a period of 2.5 years.
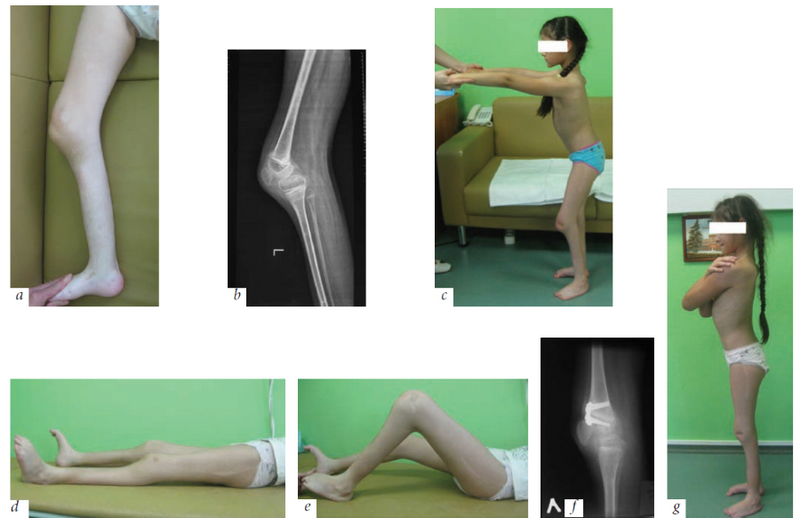
Fig. 2. Patient P., 7 years of age, with arthrogryposis with lesions of the lower limbs: a, the flexion contracture of the left knee joint of 30º and b, lateral X-ray image of the knee joint prior to treatment; c, the patient moves only with support; d, full extension, e, flexion of the knee joint up to 90º and f, lateral X-ray image 30 months after beginning treatment; g, the patient can walk independently
Comparative analysis of knee flexion contracture in patients with initial contracture ≥50° revealed that the largest correction was 90% improvement compared with the baseline value. In some patients in this group with initially more severe flexion contractures, treatment with plaster casts and a distraction device prior to surgery, achieved significantly reduced contractures. In addition to enhancing the efficiency of treatment, the use of an additional method of contracture correction reduces the treatment duration, which is very important for pediatric patients with arthrogryposis. When choosing the method of treatment of such patients it is always necessary to assess whether the functional limitations caused by flexion contracture can be tolerated during gradual correction with temporary hemiepiphysiodesis or if immediate correction is required [2]. Palocaren and Thabet (2010) recommended epiphysiodesis in patients with arthrogryposis for three years and the use of other surgical treatments of knee joint contracture continued to affect the ability to move [14]. The evidence points to the necessity to use additional methods of contracture corrections for severe knee joint contractures. With transformation into moderate or mild forms, hemiepiphysiodesis can be employed. To this end, Klatt and Stevens recommended combining temporary epiphysiodesis surgery with the recession of the tibia flexors [12]. This study included a small number of patients, and follow-up was short. More accurate evaluation of the treatment results of pediatric patients of different ages and degrees of contracture awaits performing a large prospective study.
Conclusions
Temporary hemiepiphysiodesis was effective, safe, and less invasive than other methods used to treat pediatric patients with arthrogryposis. Combining hemiepiphysiodesis with other methods of treatment allows transforming contractures from severe to moderate prior to surgery. That increases hemiepiphysiodesis effectiveness, shortens its duration, and shortens the time to achieve vertical orientation of the patient.
Information on funding and conflict of interest
The work was supported by the The Turner Scientific and Research institute for Children’s Orthopedics, Saint-Petersburg, Russian Federation. The authors declare the absence of explicit and potential conflicts of interest associated with the publication of this article.
About the authors
Svetlana I. Trofimova
The Turner Scientific and Research Institute for Children’s Orthopedics, Saint Petersburg
Author for correspondence.
Email: trofimova_sv2012@mail.ru
MD, PhD, research associate of the department of arthrogryposis Russian Federation
Dmitry S. Buklaev
The Turner Scientific and Research Institute for Children’s Orthopedics, Saint Petersburg
Email: fake@eco-vector.ru
MD, PhD, chief of the department of arthrogryposis Russian Federation
Ekaterina V. Petrova
The Turner Scientific and Research Institute for Children’s Orthopedics, Saint Petersburg
Email: fake@eco-vector.ru
MD, PhD, senior research associate of the department of arthrogryposis Russian Federation
Svetlana A. Mulevanova
The Turner Scientific and Research Institute for Children’s Orthopedics, Saint Petersburg
Email: fake@eco-vector.ru
MD, PhD student of the department of arthrogryposis Russian Federation
References
- Лапкин Ю.А., Конюхов М.П. Лечение наиболее распространенных деформаций нижних конечностей при артрогрипозе // Травматология и ортопедия России. — 2002. — № 3. — С. 86–92. [Lapkin YuA, Konyukhov MP. Lechenie naibolee rasprostranennykh deformatsii nizhnikh konechnostei pri artrogripoze. Travmatologiya i ortopediya Rossii. 2002;(3):86-92. (In Russ.)]
- Lampasi M, Antonioli D, Donzelli O. Management of knee deformities in children with arthrogryposis. Musculoskelet Surg. 2012;96(3):161-169. doi: 10.1007/s12306-012-0218-z.
- Murray C, Fixsen JA. Management of knee deformity in classical arthrogryposis multiplex congenita (amyoplasia congenita). J Pediatr Orthop B. 1997;6(3):186-191. doi: 10.1097/01202412-199707000-00006.
- MacWilliams BA, Harjinder B, Stevens PM. Guided growth for correction of knee flexion deformity: a series of four cases. Strat Traum Limb Recon. 2011;6:83-90. doi: 10.1007/s11751-011-0110-7.
- Mielke CH, Stevens PM. Hemiepiphyseal stapling for knee deformities in children younger than 10 years. J Pediatr Orthop. 1996;16:423-429. doi: 10.1097/01241398-199607000-00002.
- Al-Aubaidi Z, Lundgaard B, Pedersen NW. Anterior distal femoral hemiepiphysiodesis in the treatment of fixed knee flexion contracture in neuromuscular patients. J Child Orthop. 2012;6(4):313-318. doi: 10.1007/s11832-012-0415-1.
- van Bosse HJ, Feldman DS, Anavian J, Sala DA. Treatment of knee flexion contractures in patients with arthrogryposis. J Pediatr Orthop. 2007;27(8):930-937. doi: 10.1097/bpo.0b013e3181594cd0.
- Moreira MV, Rimoldi AC, Aoki S. Analysis on the results from percutaneous extensor osteotomy of the distal femur in patients with amyoplasia. Rev Bras Ortop. 2014;49(4):345-349. doi: 10.1016/j.rboe.2014.04.017.
- Asirvatham R, Mukherjee A, Agarwal S, et al. Supracondylar femoral extension osteotomy. J Pediatr Orthop. 1993;13(5):642-645. doi: 10.1097/01241398-199313050-00016.
- DelBello DA, Watts HG. Distal femoral extension osteotomy for knee flexion contracture in patients with arthrogryposis. J Pediatr Orthop. 1996;16:122-126. doi: 10.1097/01241398-199601000-00025.
- Eastwood DM, Sanghrajka AP. Guided growth recent advances in a deep-rooted concept. J Bone Joint Surg. 2011;93(B):12-18. doi: 10.1302/0301-620X.93B1.25181.
- Klatt J, Stevens PM. Guided growth for fixed knee flexion deformity. J Pediatr Orthop. 2008;28:626-631. doi: 10.1097/BPO.0b013e318183d573.
- Kramer A, Stevens PM. Anterior femoral stapling. J Pediatr Orthop. 2001;21(6):804-807. doi: 10.1097/01241398-200111000-00020.
- Palocaren T, Thabet AM, Rogers K, et al. Anterior distal femoral stapling for correcting knee flexion contracture in children with arthrogryposis-preliminary results. J Pediatr Orthop. 2010;30(2):169-173. doi: 10.1097/BPO.0b013e3181d07593.
- Агранович О.Е., Баиндурашвили А.Г., Петрова Е.В., и др. Консервативное лечение деформаций верхних и нижних конечностей у детей раннего возраста с артрогрипозом // Детская хирургия. — 2012. — № 2. — С. 10–15. [Agranovich OE, Baindurashvili AG, Petrova EV, et al. Konservativnoe lechenie deformatsii verkhnikh i nizhnikh konechnostei u detei rannego vozrasta s artrogripozom. Detskaya khirurgiya. 2012;(2):10-15. (In Russ.)]
- Кенис. В.М., Клычкова И.Ю., Мельченко Е.В., и др. Коррекция деформаций нижних конечностей у детей с помощью метода управляемого роста // Вестник травматологии и ортопедии им. Н.Н. Приорова. — 2013. — № 4. — С. 50–55. [Kenis VM, Klychkova IY, Melchenko EV, et al. Guided growth technique for correction of lower extremity deformities in children. Vestnik travmatologii i ortopedii im N.N. Priorova. 2013;(4):50-55. (In Russ.)]
Supplementary files









