A plantographic study of the support function of the foot in children with the malformations of the forefoot
- Authors: Nikityuk I.E.1, Kovalenko-Klychkova N.A.1
-
Affiliations:
- The Turner Scientific and Research Institute for Children’s Orthopedics, Saint Petersburg
- Issue: Vol 4, No 4 (2016)
- Pages: 77-83
- Section: Articles
- Submitted: 10.01.2017
- Accepted: 10.01.2017
- Published: 14.12.2016
- URL: https://journals.eco-vector.com/turner/article/view/5899
- DOI: https://doi.org/10.17816/PTORS4477-83
- ID: 5899
Cite item
Abstract
Full Text
Introduction
Developmental defects of the forefoot are one of the most difficult challenges in pediatric orthopedics [1, 2]. Changes in the foot affect the shape of its anterior region and impair its support function [3]. An accurate evaluation of functional parameters of the affected foot, particularly its support ability, is of critical importance. Data regarding the correlation between the foot’s support function and its geometric features are relevant while selecting a surgical treatment and designing and manufacturing corrective devices and products. Decisions regarding corrective clinical solutions are complicated by the enormous variability in what could be considered a normal foot shape for the affected foot. Therefore, the evaluation of individual morphology and function in both the pathological and unaffected foot is important. Currently, the most successful diagnostic tool for foot conditions is computer plantography [4], which considers both static and kinetostatic foot deformities in the upright position. Computer plantography reveals the severity of the deformity not only by displaying the foot loading contour but also by showing the load distribution on the various foot structures.
Despite the various plantography methods available for the assessment of pathologies of the foot, a universal method has not been established. Therefore, study of the anatomical and functional states of the feet with forefoot developmental defects in pediatric patients, through plantography, is a relevant task with significant theoretical and practical value. This is the rationale for the present study.
The study aimed to explore the morphological and functional parameters of feet in pediatric patients with developmental defects in the forefoot to assess load imbalances and to reveal the structural and functional disorders.
Material and Methods
The study of the supporting function of feet was performed using the software and hardware diagnostic complex “Podoskan” (MBN, Russia). It enabled the evaluation of morphological and functional parameters of feet in pediatric patients with developmental defects in the forefoot. Plantography characteristics were determined in 92 children aged 5–16 years, including a control group consisting of 28 healthy children (56 feet). In the group of 64 pediatric patients with a developmental forefoot defect, 30 had lesions of both feet and 34 had lesions of only one foot (right foot in 20 cases and left foot in 14). Thus, 94 feet with different localization of the anterior lesions were examined: 36 feet had lesions in the inner region, 40 feet had lesions in the median region, and 18 feet had lesions in the outer region.
To improve the method of computer plantography analysis of feet with developmental forefoot defects, the existing methods for calculating the plantography characteristics were used [5, 6], which were specifically modified for the pathology under study.
First, the calculations on the healthy children’s plantograms were performed, with identification points placed in the footprints and interconnected with lines (Fig. 1) for measuring angular and linear characteristics of the feet, as well as for calculating the plantography indices and normal coefficients.

Fig. 1. The scheme of calculating the anatomical and functional parameters of a healthy child’s foot
The scanned footprint was processed by the algorithm below. The reference points were set on the plantogram and connected with the lines:
- O – the rearmost point of the heel of the footprint,
- P – the foremost point of the V toe contour,
- Q – the foremost point of the I toe contour,
- BC – the line of the transverse arch of the foot, connecting the points B and C,;
- B – the most protruding inward point of the forefoot contour,
- C – the most protruding outward point of the forefoot contour,
- K – the point of intersection of the transverse arch line of the foot BC with the most protruding inward point of the loaded fore footprint (equivalent to the head I of the metatarsal bone),
- E – the point of intersection of the transverse line in the arch of the foot BC with the most protruding outward point of the loaded fore foot print (equivalent to the head I of the metatarsal bone),
- KE – the line of the loaded transverse arch of the foot, connecting the points K and E,
- Z – the middle of the line of the transverse arch of the foot BC,
- OZ – the notional axis of the foot,
- BN and CR – the lines drawn from points B and C parallel to the notional axis OZ of the foot,
- BP and CQ – the lines drawn from points B and C, passing through the foremost points of the V toe (P) contour and the I toe (Q) contour,
- NBP and QCR – the angle of the V toe and the I toe, respectively,
- ОG, ОD, ОS, ОW, and ОH – Dyukendzhiev’s lines – 1, 2, 3, 4, and 5 (power rays of load direction to I, II, III, IV, and V toes respectively),
- G, D, S, W, and H – points of intersection of the corresponding Dyukendzhiev’s lines – 1, 2, 3, 4, and 5 with the front edge of the fore footprint,
- G1, D1, S1, W1, and H1 – points of intersection of the corresponding Dyukendzhiev’s lines – 1, 2, 3, 4, and 5 with the line of the transverse arch of the foot BC,
- U – the intersection point of the Dyukendzhiev’s line - 1 with the rear contour line of the print of the anteromedial part of the foot,
- Х – the intersection point of the Dyukendzhiev’s line - 2 with the rear contour line of the print of the median region of the foot,
- A – the center of the heel print,
- LM – the line intersecting the center A and the edges of the heel print in the widest place, that is in the points L and M.
The plantography indexes were calculated, which were used for the characterization of normal foot prints and for all the defects of the forefoot:
- KE/BC – load capacity index of the forefoot, which reflects the completeness of the load on the forefoot,
- LM/KE – the Chipaux–Smirak index which shows the load distribution between the forefoot and the rearfoot.
Furthermore, for the characterization of feet combined in groups with localization of lesions in the forefoot, the additional indices and coefficients were calculated:
For the defect of the inner region of the forefoot
- GU/GO – the ray I support index, which reflects the support ability of the head I of the metatarsal bone,
- k1 = GG1: 1/5OZ – the coefficient of the distal support of the ray I for detection of displacement of the front contour of the spot of the metatarsal bone support I;
For the defect of the median region of the forefoot:
- DX/DO – the support index of the median region, which reflects the support ability the metatarsal bone heads II-III,
- k2 = DD1: 1/5OZ – the coefficient of the distal support of the ray II for detection of displacement of the front contour of the spot of the metatarsal bone support II,
- k3 = SS1: 1/5OZ – the coefficient of the distal support of the ray III for detection of displacement of the front contour of the spot of the metatarsal bone support III,
- k4 =WW1: 1/5OZ – the coefficient of the distal support of the ray IV for detection of displacement of the front contour of the spot of the metatarsal bone support IV,
- k2-3-4 = 1/3 × (K2 + K3 + K4) – the average coefficient of the distal support of the median rays for evaluation of the deformity of the front contour of the spot of the median foot part support;
For the defect of the outer region of the forefoot:
- k5 = НН1: 1/5OZ – the coefficient of the distal support of the ray V for detection of displacement of the front contour of the spot of the metatarsal bone support V.
Statistical analysis of the study results was conducted using Microsoft Excel, including calculation of the mean variation series M, mean-square deviation m and 95% confidence interval. The threshold level of statistical significance was taken at the value of the criterion p < 0.05.
Results
In the patients with forefoot developmental defects, the plantograms were divided into three groups, depending on the lesion location, with the corresponding identification points set with subsequent connections between lines, and the angular and linear characteristics of the feet were calculated (Fig. 2).
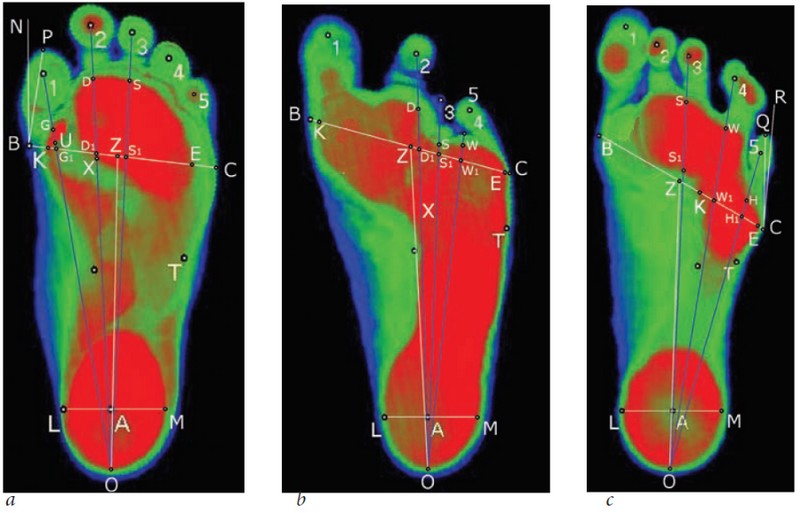
Fig. 2. The scheme of calculation of the anatomic and functional parameters of the patients’ feet with developmental defects of the forefoot, depending on the lesion location: a) the defect of the inner region; b) the defect of the median region; c) the defect of the outer region
Plantography characteristics in children with forefoot developmental defects, specific to location of the lesion, are presented in Table 1. Analysis of the table showed that the average value of the forefoot load capacity index in healthy children was 94.7% ± 0.39%. In patients with forefoot developmental defects the average value of this index decreased significantly, up to 71.6% ± 1.55% in the location of pathology in the inner region; up to 74.0% ± 1.57% where pathology was found in the median region, and up to 78.6% ± 2.04% in cases where pathology was in the outer region (p < 0.05).
Table 1. Comparative assessment of plantography characteristics of healthy children’s feet and those of patients who have forefoot developmental defects, categorized by lesion location (M ± m)
Parameters | Healthy children (n = 56) | Patients with the forefoot developmental defect | ||
Defect of the inner region (n = 36) | Defect of the median region (n = 40) | Defect of the outer region (n = 18) | ||
Load capacity index of the forefoot, % | 94.7 ± 0.39 | 71.6 ± 1.55* | 74.0 ± 1.57* | 78.6 ± 2.04* |
Chipaux–Smirak index | 0.53 ± 0.006 | 0.79 ± 0.024* | 0.75 ± 0.023* | 0.63 ± 0.022* |
Coefficient of the distal support I of the ray k1 | 0.70 ± 0.01 | 0.27 ± 0.02* | – | – |
Support index of the ray I (× 10−2) | 23.3 ± 0.44 | 11.7 ± 1.01* | – | – |
Angle of the toe I, ° | 12.0 ± 0.48 | –0.03 ± 1.32* | – | – |
Coefficient of the distal support II of the ray k2 | 0.99 ± 0.01 | – | 0.78 ± 0.02* | – |
Coefficient of the distal support III of the ray k3 | 0.97 ± 0.02 | – | 0.65 ± 0.03* | – |
Coefficient of the distal support IV of the ray k4 | 0.81 ± 0.01 | – | 0.42 ± 0.02* | – |
Average coefficient of the distal support II, III, IV of the rays k2-3-4 | 0.92 ± 0.01 | – | 0.62 ± 0.02* | – |
Support index of the median region (× 10–2) | 24.5 ± 0.32 | – | 22.4 ± 0.48* | – |
Coefficient of the distal support V of the ray k5 | 0.54 ± 0.01 | – | – | 0.26 ± 0.04* |
Angle of the toe V, ° | 13.4 ± 0.52 | – | – | –2.5 ± 1.62* |
* The values varied significantly from the nor, with accuracy of at least p < 0.05.
Thus, in patients with developmental defects of the forefoot, the load distribution in this region was uneven; therefore, the deficit of the forefoot support capability was considerable: 32%, 28%, and 20% for the defects of inner, median, and outer regions, respectively.
Addition of the Chipaux–Smirak index to the analysis of plantograms provides insight into nature of the load displacement on the different regions of the foot. Thus, if the ratio of load on the rearfoot to the load on the forefoot is 0.53 ± 0.006 in healthy pediatric patients, then in patients with a forefoot defect the Chipaux–Smirak index was increased to 0.79 ± 0.024 with the localization of pathology in the inner region, 0.75 ± 0.023 with the localization of pathology in the median region, and 0.63 ± 0.022 with the localization of pathology in the outer region (p < 0.05).
Thus, in patients with a forefoot developmental defects, the “calcaneusation” of the plantar load occurs, namely significant displacement of the support capability from the forefoot to the rearfoot on the calcaneus: with a surplus of 49% in case of pathology localized to the inner region; 42% in cases with pathology localized to the median region; and 19% in cases of pathology localized to the outer region. The most significant increase in the Chipaux–Smirak index was detected in patients with deformities in the inner and median regions. This indicates that, with this localization of pathology, the load distribution in the forefoot is so significantly impaired that it causes a combined load displacement both within the forefoot and posteriorly. This leads to long-term inadequate overload of some parts of the foot and lack of load in other parts of the foot, which is the cause of impairment of the statnamic foot function in both cases.
The use of additional indexes and coefficients enabled more detailed assessment of impairment of the foot function, depending on the localization of the pathology in the forefoot.
The developmental defect of the inner region of the forefoot (Fig. 2, a). In the group of patients with this pathology the support index of ray I appeared to be reduced by two times, up to (11.7 ± 1.01) × 10−2 compared to that of the healthy children, which was (23.3 ± 0.44) × 10-2 (p < 0.05). Also, the patients showed a 2.6 times decrease of the coefficient of the distal support I of the ray k1 to 0.27 ± 0.02, as compared with this parameter in healthy children: 0.70 ± 0.01 (p < 0.05). In the observed group of patients the angle of the toe I was also significantly reduced, which was to −0.03° ± 1.32° compared to the same index in the norm: 12.0° ± 0.48° (p < 0.05).
Thus, in patients with the forefoot developmental defects with pathology localized to the inner region there is a significant deviation from the norm in plantography characteristics, which indicates the uneven load distribution on the foot regions, rough rear displacement of the inner point of the foot support, the load deficit on the head I of the metatarsal bone.
The developmental defect of the median region of the forefoot (Fig. 2, b). In this pathology localization, though the parameters of the plantography characteristics were not drastically deviated from the norm, they were statistically significantly and consistently reduced. The support index on the median region of the foot was slightly reduced: by 9% - up to (22.4 ± 0.48) × 10-2 compared to the healthy children (24.5 ± 0.32) × 10-2 (p <0.05). Much more indicative values were the consistently low values of the coefficients of the distal support II, III, and IV of rays: k2, k3, and k4, with a reduction magnitude of 27%, 49%, and 93% respectively. It is noteworthy that the smallest deviation from the norm is observed in the coefficient k2, while the highest deviations are observed in the coefficients k3 and especially k4. This is due to a large proportion of patients with such forms of nosology as brachymetatarsia with shortening of either one (usually IV) or two (III and again IV) metatarsals. An average rearward displacement of the front contour of the median region of the foot is characterized by a coefficient k2-3-4, which was reduced in the patients by 48% as compared with the healthy children: 0.62 ± 0.02 and 0.92 ± 0.01, respectively (p < 0.05).
Thus, in patients with forefoot developmental defects with the pathology localized to the median region, there is a deformity of the distal contour of the foot median region support with a significant displacement anterior to the loaded zone, especially in the projection of the heads III and IV of the metatarsal bones. At the same time there is the uneven load distribution on the foot regions, which indicates the impairment of its support function.
The developmental defect of the outer region of the forefoot (Fig. 2, c). The analysis of additional plantography characteristics in the group of patients with the said pathology revealed a significant deviation from the norm of linear and angular parameters of the footprints. The coefficient value of the distal support V of the ray k5 in this group of patients was significantly reduced: by 108% to 0.26 ± 0.04 compared to the normal value of 0.54 ± 0.01 (p < 0.05). The angle of the toe V was significantly reduced: up to −2.5° ± 1.62° compared with the normal value of this angle of 13.4° ± 0.52° (p < 0.05).
Thus, in patients with forefoot developmental defects with the localization of pathology in the outer region there is significant deviation from the norm of the plantography characteristics, indicating the uneven load distribution on the foot regions, pronounced posterior displacement of the outer point of the foot support, and lateralization of the distribution of the forefoot support capability.
Discussion
The plantography data showed that in patients with forefoot developmental defects, a significant deviation from the norm of plantography characteristics from 10% to 150% is noted. The extent of disorder in pathological foot parameters is reasonable to compare with the parameters of physiological changes in the normal foot. It is known that in the vertical position in the healthy body, weight is distributed on the forefoot as 20.5% for the anterior-inner region, and nearly the same amount for the anteroexternal region, which is 18.5% [7]. When walking, the load on the forefoot increases to a greater extent due to the inner region, that is up to 36%, and the contribution of the outer region is 26% [8]. That is, under normal load on the foot in the normal the variation of the load parameters in the forefoot is in the range of 10-15%, while in case of forefoot developmental defect the amount of the load distribution changes reaches 32%. This impairment of normal load ratio on different regions of the foot leads not only to the impairment of its functions [9], but also to the deformity of the musculoskeletal system and the impairment of various body functions.
Impairment of length proportions of the foot rays inevitably has an impact on walking, for which there is a certain, fixed sequence of contact of the foot regions with the support. In the phase of rolling through the forefoot the region of the metatarsal head V is the first which comes into contact with the support, followed by the region of the heads, II, III, IV of the metatarsal bones, and the region of the head I of the metatarsal bone completes the contact. That is, the rolling of the foot in the forefoot occurs in the frontal plane [10], and this is the most dynamically loadable process along with the rolling through the heel. The plantography data analysis showed that in case of the forefoot developmental defect there is a significant displacement of the front support points of the foot in the sagittal plane, which leads to deformity of the foot rolling path in the frontal plane. This in turn causes the disturbance of spatial, temporal, kinematic, and dynamic parameters of the step cycle [11].
Conclusions
- The proposed method of analysis of foot prints in cases of forefoot developmental defects has a high chance of resolution and allows for specification and identification of the nature of pathologies within the foot support function, characterized by location of the lesion.
- A foot with the forefoot developmental defect is a single functional unit, and the location of the pathological process in any region (inner, median or outer) has an integrative effect on its support function, which leads to disruption of biomechanics, not only of individual regions but of the entire foot. The most pronounced deviations of the reference function of the foot were revealed with the location of lesion in the inner region of the forefoot, while the less pronounced deviations were seen in pathologies of the outer region.
- The nature of these deviations indicate the impairment of foot statics (support function) and the inferiority of its dynamic function (the impairment of the rolling phase through the forefoot when walking), which indicates the appropriateness of the surgical repair of foot anatomy to improve its function.
About the authors
Igor E. Nikityuk
The Turner Scientific and Research Institute for Children’s Orthopedics, Saint Petersburg
Author for correspondence.
Email: femtotech@mail.ru
MD, PhD, leading research associate of the laboratory of physiological and biomechanical research Russian Federation
Nadezhda A. Kovalenko-Klychkova
The Turner Scientific and Research Institute for Children’s Orthopedics, Saint Petersburg
Email: fake@eco-vector.com
MD, orthopedic surgeon of the department of foot pathology, neuroorthopedics and systemic diseases Russian Federation
References
- Capobianco CM. Surgical treatment approaches to second metatarsophalangeal joint pathology. Clin Podiatr Med Surg. 2012;293:443-9.
- Smolle E, Scheipl S, Leithner A, Radl R. Management of congenital fourth brachymetatarsia by additive autologous lengthening osteotomy (AALO): a case series. Foot Ankle Int. 2015;36(3):325-9. doi: 10.1177/1071100714557520.
- Конюхов М.П., Клычкова И.Ю., Коваленко-Клычкова Н.А., Никитюк И.Е. Пороки развития первого луча стопы у детей: диагностика, клиника, лечение // Ортопедия, травматология и восстановительная хирургия детского возраста. — 2015. — Т. 3. — Вып. 2. — С. 15–24. [Konyukhov MP, Klychkova IY, Kovalenko-Klychkova NA, Nikityuk IE. Malformations of the first ray of the foot in children: diagnosis, clinical picture, treatment. Pediatric traumatology, orthopaedics and reconstructive surgery. 2015;3(2):15-24. (In Russ.)]
- Dzieciol Z, Kuryliszyn-Moskal A, Dzieciol J. Application of plantography examination to the assessment of foot deformity in patients with rheumatoid arthritis. Arch Med Sci. 2015;11(5):1015-1020.
- Перепелкин А.И., Мандриков В.Б., Краюшкин А.И. Влияние дозированной нагрузки на изменение структуры и функции стопы человека: Монография. — Волгоград: Изд-во ВолгГМУ, 2012. — 182 c. [Perepelkin AI, Mandrikov VB, Krayushkin AI. Vliyanie dozirovannoi nagruzki na izmenenie struktury i funktsii stopy cheloveka: Monografiya. Volgograd: Izd-vo VolgGMU; 2012. 182 p. (In Russ.)]
- Никитюк И.Е., Клычкова И.Ю. Компьютерная плантография как метод диагностики врожденной косолапости у детей // Ортопедия, травматология и восстановительная хирургия детского возраста. — 2015. — Т. 3. — Вып. 3. — С. 26–31. [Nikityuk IE, Klychkova IY. Computer plantography as a diagnostic method for congenital clubfoot in children. Pediatric traumatology, orthopaedics and reconstructive surgery. 2015;3(3):26-31. (In Russ.)]
- Кашуба В.А. Биомеханика осанки. — Киев: Олимпийская литература, 2003. — 279 с. [Kashuba VA. Biomekhanika osanki. Kiev: Olimpiiskaya literature; 2003. 279 p. (In Russ.)]
- Давыдов В.Ю. Проблемы внедрения соматотипирования в диагностику морфофункциональных состояний опорно-двигательного аппарата спортсменов // Мат. междунар. науч.-практ. конф. «Проблемы диагностики, укрепления и реабилитации опорно-двигательного аппарата у спортсменов». — Волгоград: ФГОУ ВПО «ВГАФК», 2008. — С. 45–46. [Davydov VYu. Problemy vnedreniya somatotipirovaniya v diagnostiku morfo-funktsional’nykh sostoyanii oporno-dvigatel’nogo apparata sportsmenov. (conference proceedings) Mat. mezhdunar. nauch.-prakt. konf. “Problemy diagnostiki, ukrepleniya i reabilitatsii oporno-dvigatel’nogo apparata u sportsmenov”. Volgograd: FGOU VPO “VGAFK”; 2008. P. 45-46. (In Russ.)]
- Murphy DF, Beynnon BD, Michelson JD, Vacek PM. Efficacy of plantar loading parameters during gait in terms of reliability, variability, effect of gender and relationship between contact area and plantar pressure. Foot ankle Int. 2005;26(2):171-179.
- Скворцов Д.В. Диагностика двигательной патологии инструментальными методами: анализ походки, стабилометрия. — М.: Т.М. Андреева, 2007. — 640 с. [Skvortsov DV. Diagnostika dvigatel’noi patologii instrumental’nymi metodami: analiz pokhodki, stabilometriya. Moscow: T.M. Andreeva; 2007. 640 p. (In Russ.)]
- Perry J. Gait analysis. Normal and pathological function. SLACK Incorporated; 1992. 524 p.
Supplementary files









