The use of a synthetic analogue of prostaglandin Е1 misoprostol for induction of labor
- Authors: Blagodarniy G.V1
-
Affiliations:
- FSBSI “The Research Institute of Obstetrics, Gynecology and Reproductology named after D.O. Ott”
- Issue: Vol 66, No 1 (2017)
- Pages: 56-65
- Section: Articles
- Submitted: 15.01.2017
- Published: 15.01.2017
- URL: https://journals.eco-vector.com/jowd/article/view/6096
- DOI: https://doi.org/10.17816/JOWD66156-65
- ID: 6096
Cite item
Full Text
Abstract
Keywords
Full Text
На данном этапе развития акушерства проблема индукции родов остается особенно актуальной ввиду наличия большого количества показаний к данному вмешательству, а также высокой частоты индукции родов. Данный факт диктует необходимость поиска наиболее безопасного и эффективного метода родовозбуждения.
Все методы родовозбуждения могут быть разделены на механические и медикаментозные. К механическим методам относят такие манипуляции, как амниотомия, применение интрацервикального введения катетера Фолея, интрацервикальное введение ламинарий, отслаивание плодных оболочек. К медикаментозным методам стоит отнести применение различных лекарственных форм простагландинов семейства Е и F, введение окситоцина [1, 2].
В последние годы большое количество клинических исследований посвящено применению простагландинов для родовозбуждения.
Простагландины являются биологически активными веществами, синтезируемыми эндогенно из арахидоновой кислоты, которая поступает в организм с пищей или может быть синтезирована de novo из полиненасыщенных жирных кислот. Из арахидоновой кислоты формируются предшественники простагландинов — эйкозаноиды, которые в дальнейшем путем ферментации в тканях превращаются в активные тканеспецифические метаболиты. Простагландины являются биологически активными веществами, обладающими паракринным механизмом действия, то есть являются локальными биорегуляторами [3].
Среди большого количества простагландинов особый интерес для практического акушерства представляют простагландины Е 1, Е 2 и F2α. Они являются тканеспецифическими биорегуляторами для миометрия матки человека, воздействие их с миоцитами приводит к развитию сокращения или расслаблению в клетках миометрия. Механизм сокращения клеток миометрия под воздействием простагландинов схематически представлен на рис. 1 [4].
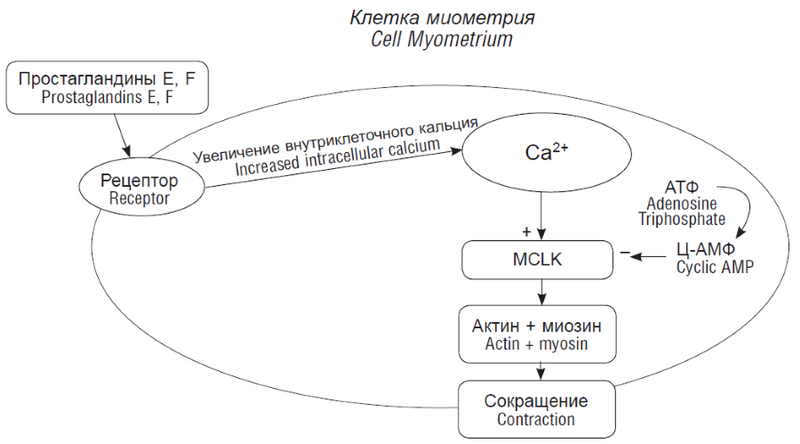
Рис. 1. Механизм сокращения клетки миометрия
Fig. 1. The mechanism of reducing the myometrium cells
Начальным и определяющим моментом сокращения миометрия является связывание ионов Са2+ с кальмодулином. Комплекс Са2+ — кальмодулин приводит к активации специфического для гладких мышц фермента — миозин-легкоцепочечной киназы (MCLK). Миозин-легкоцепочечная киназа является ключевым ферментом сокращения миометрия [4]. Этот энзим приводит к фосфорилированию легких цепей миозина, в ответ на это миозин гидролизует АТФ до АДФ и начинает связываться с актином, меняется конформация миозина и происходит скольжение нитей миозина вдоль нитей актина, что приводит к сокращению миоцитов и развитию родовой деятельности.
Свое биологическое действие простагландины Е1 и Е2 реализуют через связывание со специфическими рецепторами, экспрессируемыми на клетках миометрия. Так, при связывании молекулы простагландинов Е с рецепторами EP1 и ЕР3 открывается мембранный канал для ионов кальция, что приводит к увеличению концентрации внутриклеточного кальция и, как следствие, к сокращению миометрия [5].
При связывании лиганда простагландинов Е со специфическими рецепторами типов EP2 и EP4 происходит активация аденилат-циклазной системы, увеличивается концентрация ц-АМФ, что приводит к расслаблению миометрия. При изучении плотности распространения рецепторов к простагландинам на клетках миометрия было показано, что «сократительные» рецепторы типов EP1 и ЕР3 преимущественно располагаются в дне матки, а «расслабляющие» рецепторы типов ЕP2 и ЕР4 — в нижнем сегменте матки [5]. Таким образом, можно предположить, что назначение простагландина Е 1 с целью индукции родов является физиологически обоснованным методом родовозбуждения.
В нашем обзоре представлены данные исследований об индукции родов с помощью синтетического аналога простагландина Е1 — мизопростола.
Как было показано выше, простагландин Е1 является тономоторным агентом, образующимся in vivo. Это его свойство вызвало большой интерес исследователей и практикующих врачей к оценке его эффективности и безопасности, разработке схем родовозбуждения и изучения его эффективности при различных путях введения. Первые публикации, посвященные этому вопросу, датируются 1999 г., однако по настоящее время проводятся исследования эффективности и безопасности родовозбуждения мизопростолом. Существуют различные пути введения мизопростола — вагинальный, трансбуккальный, сублингвальный, ректальный. В современной литературе нами не было обнаружено исследований, в достаточной мере оценивающих влияние мизопростола при трансбуккальном, ректальном и сублингвальном введении. Трансбуккальное, ректальное и сублингвальное введение мизопростола почти не используется в клинической практике, поскольку были получены данные о неблагоприятных эффектах, наиболее частый из которых — гиперстимуляция матки. Наиболее изученными являются пероральный и трансвагинальный пути введения синтетического аналога простагландина Е1.
Фармакокинетика мизопростола была исследована в работе Ziman et al. в 1997 г. [6]. Сравнивался вагинальный и оральный пути введения препарата. Вводили 400 мкг мизопростола. По результатам исследования выявлено, что после перорального приема мизопростола концентрация мизопростоловой кислоты в плазме нарастает быстро и постепенно снижается после 120 минут. Пиковая концентрация достигается через 34 ± 17 мин. После вагинального введения препарата концентрация активного метаболита в плазме растет постепенно и медленно снижается к 240-й минуте. Пиковая концентрация мизопростоловой кислоты в плазме достигалась через 80 ± 27 мин. Через 6 ч после перорального введения концентрация в плазме составила 303 ± 103,3 пг в ч/мл, тогда как после вагинального введения этот показатель составил 956,7 ± 541,7 пг в ч/мл. Таким образом, биодоступность препарата при вагинальном введении выше, однако эффект индивидуален, что обусловлено значительными колебаниями концентрации препарата в плазме (956,7 ± 541,7 пкг/мл). Другие исследования [7] показали, что pH влагалища не влияет на биодоступность препарата, также было показано, что размачивание таблетки мизопростола в воде также не приводит к увеличению его биодоступности.
Кривые фармакокинетики мизопростола представлены на рис. 2 [6].
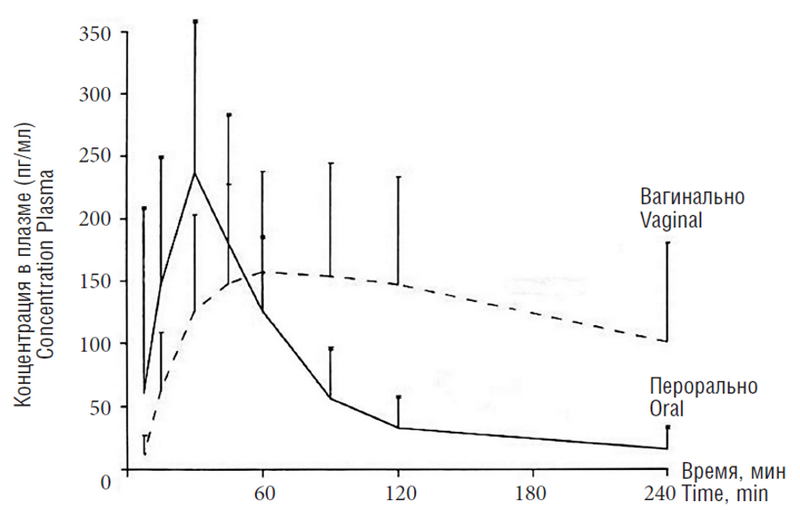
Рис. 2. Концентрация мизопростола в плазме крови при пероральном и вагинальном введении
Fig. 2. Misoprostol concentration in blood plasma by oral and vaginal administration
В 1999 г. был опубликован первый метаанализ [8], посвященный оценке эффективности индукции родов с применением мизопростола. Основными выводами стали следующие: вагинальное применение мизопростола показало высокую эффективность (в течение 24 ч родоразрешены 89,3 % беременных), было более эффективным, чем применение окситоцина, однако риск гиперстимуляции матки, наоборот, был выше при применении мизопростола. Пероральное введение мизопростола также было эффективным (87,4 %), интервал от начала родовозбуждения до родов был меньше, чем при применении других методов родовозбуждения. При сравнении перорального и вагинального введения аналога простагландина Е1 не было выявлено статистических различий в особенностях течения родов и побочных эффектах. Однако авторы отметили, что требуются дополнительные исследования.
В 1999 г. американскими исследователями под руководством D. Wing [9] проведено сравнение эффективности индукции родов при вагинальном введении 25 мкг мизопростола каждые 4 ч и перорального введения 50 мкг мизопростола каждые 4 ч. Была показана меньшая эффективность перорально применяемого мизопростола в сравнении с вагинальным. В течение 24 ч в первой группе были родоразрешены 52,4 % пациенток, тогда как во второй — только 32,3 %. Интервал до начала родовозбуждения при пероральном применении 50 мкг мизопростола был на 6 ч больше, чем при его вагинальном введении. Несмотря на это, через естественные родовые пути были родоразрешены 86,4 % пациенток из второй группы и 77,3 % из первой. Различий по частоте возникновения тахисистолии матки между группами отмечено не было.
Однако в 2009 г. [10] при сравнении малых доз мизопростола (20 мкг перорально каждые 4 ч и 25 мкг мизопростола вагинально каждые 4 ч) не было отмечено статистических различий в количестве акушерских осложнений родов, частоты кесарева сечения и эффективности родовозбуждения, частоты гипоксии плода. При этом гиперстимуляция матки достоверно чаще встречалась при вагинальном введении (2 и 13 % соответственно).
Противоречивые данные получены в двух исследованиях, проведенных в 2013 г. В первом из них, проведенном Deshmukl et al. в Индии, 200 женщин были разделены поровну [11], сравнивали индукцию родов при пероральном введении 50 мкг мизопростола и при вагинальном введении 50 мкг мизопростола. Интервал между введениями составил 6 ч. Время до начала родовой деятельности при вагинальном применении мизопростола было достоверно меньшим (12,74 + 2,6 ч) по сравнению с пероральным применением (15,24 + 3,47 ч). Слабость родовой деятельности достоверно (p < 0,05) реже встречалась при вагинальном введении. Кесарево сечение в связи с неэффективным родовозбуждением выполнено в 26 и 17 случаев соответственно. Сделан вывод о предпочтительности вагинального введения 50 мкг мизопростола.
В исследовании Komala [12], в которое вошли 200 женщин, оценивалось родовозбуждение при вагинальном применении препарата (25 мкг каждые 4 ч) и пероральном применении (50 мкг каждые 6 часов). Среднее время от начала родовозбуждения до родов не различалось статистически и составило 12,92 ч при вагинальном применении и 14,04 ч при пероральном. Не было найдено различий в частоте слабости родовой деятельности, частоте оперативного родоразрешения и неонатальных исходов. Однако была подтверждена гипотеза о том, что дискоординация родовой деятельности реже возникает при пероральном применении мизопростола (2,7 % при пероральном и 14,4 % при вагинальном применении).
На основании исследований, посвященных вопросу индукции родов, были проведены кохрейновские обзоры и метаанализы. В феврале 2015 г. [13] Кохрейновской группой по беременности и родам опубликован метаанализ, посвященный использованию простагландинов для индукции родов. В обзор были включены 280 исследований (48 068 пациенток). Основной вывод метаанализа: мизопростол является эффективным и безопасным препаратом, применяемым для индукции родов, и позволяет считать его лучшим современным препаратом для медикаментозного родовозбуждения. При использовании низких доз мизопростола перорально при разведении (менее 50 мкг) вероятность кесарева сечения наиболее низкая, тогда как при вагинальном применении мизопростола (в дозе 50 и более мкг) частота родоразрешения через естественные родовые пути в течение 24 ч от начала родовозбуждения самая высокая.
В большинстве исследований была показана высокая эффективность мизопростола как средства индукции родов.
Большое внимание уделяется индукции родов при помощи перорального введения мизопростола при разведении (в англоязычной литературе titrated misoprostol for labor induction). Этот метод позволяет снизить дозу мизопростола.
В последние годы были опубликованы результаты нескольких исследований, целью которых явилась оценка эффективности и безопасности родовозбуждения при пероральном введении мизопростола при разведении, а также в сравнении с другими методами родовозбуждения. Так, в работе Cheng et al. 2010 г. [14] исследовались исходы родов при применении раствора мизопростола у первородящих и повторнородящих. Был проведен ретроспективный анализ историй родов у женщин с доношенным сроком беременности. В данном исследовании женщины получали перорально по 20 мкг мизопростола каждый час в течение 4 ч. По результатам исследования в течение 12 ч от начала родовозбуждения были родоразрешены через естественные родовые пути 42,9 % первородящих и 85,7 % повторнородящих, однако не наблюдалось случаев безуспешного родовозбуждения. При анализе течения родов гиперстимуляции и гипертонуса матки отмечено не было, однако отмечалась тахисистолия матки у 8 % первородящих и 6 % повторнородящих. Все дети родились с оценкой по шкале Апгар 7 баллов и более.
В 2008 г. проведено рандомизированное контролируемое исследование, в которое были включены 220 рожениц. Сравнивали индукцию родов путем перорального введения раствора мизопростола и вагинального введения препарата [15]. Применяли раствор мизопростола (доза препарата составила 25 мкг мизопростола каждые 4 ч) и вагинальное введение 25 мкг мизопростола каждые 4 ч до наступления активной родовой деятельности. В результате было отмечено достоверное различие между временным интервалом от начала индукции родов до родоразрешения, который составил 8,2 ч при пероральном применении мизопростола и 17,6 ч при вагинальном. Не было отмечено значимых различий при анализе таких осложнений родового акта, как тахисистолия, гипертонус матки и снижение амплитуды осцилляций и акцелераций, по данным кардиотокографии при различных путях введения препарата. Так, тахисистолия возникла в 6,9 и в 15,6 % наблюдений соответственно. Однако при вагинальном применении мизопростола в ряде случаев была отмечена гиперстимуляция матки, тогда как при пероральном применении препарата такого осложнения зафиксировано не было. Исследователи объясняют это тем, что при пероральном введении раствора мизопростола в любой момент может быть прекращено поступление препарата в системный кровоток, то есть такой метод введения является более контролируемым и удобным. Кесарево сечение было выполнено у 4,0 и 17,0 % (p < 0,01) рожениц соответственно.
При оценке состояния новорожденных не отмечено случаев возникновения асфиксии в родах при пероральном введении мизопростола, тогда как при вагинальном применении была отмечена асфиксия легкой степени в 5,7 % наблюдений. Таким образом, пероральный путь введения мизопростола является более безопасным, так как при разведении достигнут достоверно меньший уровень абдоминального родоразрешения, а также реже наблюдаются такие осложнения, как тахисистолия матки, дискоординация родовой деятельности.
В 2013 г. проведено тройное слепое рандомизированное многоцентровое исследование A.S. Souza et al. [16], целью которого являлось сравнение эффективности и безопасности перорального введения мизопростола при разведении и вагинального введения мизопростола. В исследование были включены 200 первородящих. Перорально вводили раствор мизопростола в дозе 20 мкг в час, затем дозу увеличивали на 20 мкг каждые 6 ч. Вагинально вводили 25 мкг мизопростола каждые 6 ч. Значимых различий найдено не было. Частота отсутствия эффекта от родовозбуждения, необходимости применения окситоцина была одинаковой. Осложнения родового акта (такие как тахисистолия и гиперстимуляция матки), перинатальные исходы также были одинаковыми как при пероральном введении раствора мизопростола, так и при вагинальном его введении. 70 % женщин предпочли пероральное введение мизопростола.
Один из наиболее важных выводов в приведенных исследованиях заключается в том, что интервал от начала родовозбуждения до появления схваток был более коротким при пероральном применении раствора мизопростола. Дробное введение препарата позволяет минимизировать дозу вводимого препарата, то есть сделать процесс родовозбуждения более контролируемым.
Внимания также заслуживают данные исследований, в которых проводился сравнительный анализ эффективности и безопасности индукции родов мизопростолом и других методов родовозбуждения.
Мизопростол и динопростон
В 2006 г. Crane и Butler опубликовали систематический обзор, в котором проводилась оценка эффективности и безопасности родовозбуждения при доношенном сроке беременности у женщин с целым плодным пузырем и незрелой шейкой матки [17] на основании 611 статей. Целью данной работы была оценка частоты кесарева сечения при отсутствии эффекта от родовозбуждения, а также оценка частоты осложнений родов. На первом этапе сравнивались различные пути введения и дозы исследуемых препаратов. Достоверных различий по частоте оперативного родоразрешения между мизопростолом и динопростоном не было, однако при использовании мизопростола наблюдалась более высокая частота тахисистолии и гиперстимуляции матки вне зависимости от пути доставки препарата. Была отмечена более высокая частота родов через естественные родовые пути в течение 24 ч после начала родовозбуждения при вагинальном пути введения мизопростола по сравнению с простагландином Е2. Кроме того, у женщин, получивших индукцию родов мизопростолом, реже применялась родостимуляция окситоцином. Таким образом, более эффективным оказалось применение мизопростола с целью индукции родов, чем применение динопростона. При этом частота кесарева сечения не различалась при обоих методах индукции родов.
В работе английских акушеров под руководством Ozkan (2009) [18] были получены несколько другие данные. При сравнении эффективности мизопростола (50 мкг интравагинально каждые 4 ч) и динопростона (интравагинально 10 мг через 12 ч) у женщин с незрелой шейкой матки при доношенном сроке беременности достоверно показано, что интервал от начала родовозбуждения до родов был значительно меньше при применении мизопростола (680 мин по сравнению с 1070 мин при применении динопростона). При применении мизопростола родоразрешение через естественные родовые пути в течение 12 ч наступало значительно чаще (66 % случаев при применении мизопростола и 42 % случаев при применении динопростона). Кроме того, показано, что назначение окситоцина требовалось чаще в группе динопростона. При этом авторы не нашли значительных различий в частоте гиперстимуляции матки, чрезмерной родовой деятельности и неблагоприятных последствий для плода при применении обоих простагландинов.
В 2013 г. в работе Petersen были получены следующие данные. При сравнении вагинального введения 25 мкг мизопростола однократно и 6 мг динопростона однократно отмечено, что в группе, в которой применялся простагландин Е 1, интервал от начала родовозбуждения до родоразрешения был более продолжительным, чем при применении динопростона. Не было различий в частоте асфиксии новорожденных, появлении мекония в околоплодных водах [19].
Таким образом, данные исследований противоречивы. Основные результаты исследований представлены в табл. 1.
Таблица 1. Сравнение мизопростола и динопростона для индукции родов
Table 1. Comparison of misoprostol and dinoprostone for induction of labor
Автор | Год | Тип исследования | Сравниваемые методы родовозбуждения | Основные результаты |
Crane | 2006 | Систематический анализ 611 публикаций | Мизопростол и динопростон | Мизопростол более эффективен для индукции родов, чем динопростон. Частота дискоординированных схваток при применении динопростона меньше |
Ozkan | 2009 | Клиническое исследование | Вагинальный мизопростол и динопростон | Интервал от начала индукции до начала схваток более короткий при применении мизопростола. Потребность в применении окситоцина больше при применении динопростона |
Petersen | 2013 | Клиническое исследование | Низкие дозы мизопростола вагинального и динопростон | Интервал до начала схваток более продолжителен при применении мизопростола. Нет различий в перинатальных исходах в обеих группах |
Мизопростол и интрацервикальное введение катетера Фолея и инфузия окситоцина
В 1999 г. опубликована работа D. Abramovici et al. [20], в которой сравнивались оральное введение мизопростола (по 50 мкг каждые 4 ч) и одновременное применение катетера Фолея и окситоцина. В исследование вошли 200 пациенток с недостаточно зрелой шейкой матки, которые требовали родовозбуждения. У повторнородящих женщин различий в параметрах индукции родов и течении родового акта выявлено не было. У первородящих женщин при применении мизопростола родоразрешение в течение 24 ч наступало реже и средний интервал от начала родов до родоразрешения был больше (23,3 ч при применении мизопростола и 17,2 ч при применении катетера Фолея и окситоцина). Не было различий в оценке по шкале Апгар, частоте оперативного родоразрешения и появления хориоамнионита. Авторы делают вывод о том, что мизопростол так же эффективен, как и окситоцин.
Эти результаты были подтверждены в опубликованном в 2004 г. исследовании [21] Culver. Исследовалось применение катетера Фолея и вагинального введения мизопростола у первородящих с недостаточно зрелой шейкой матки. Среди 162 пациенток, включенных в исследование, 79 получали 25 мкг мизопростола интравагинально каждые 4 ч, а 83 пациенткам интрацервикально введен катетер Фолея с одновременной внутривенной инфузией окситоцина. Статистических различий по частоте кесарева сечения, связанного с неэффективностью родовозбуждения, не выявлено (35 % при применении мизопростола и 29 % при применении катетера Фолея). Не было также статистических различий по частоте осложнений родового акта, послеродового периода, неблагоприятных исходов для новорожденных. Единственным отличием, как и в предыдущем исследовании, была продолжительность интервала «родовозбуждение — роды», которая составила 18 ч при совместном применении интрацервикального баллона и окситоцина и 24 ч при вагинальном введении 25 мкг мизопростола.
В 2010 г. проведено рандомизированное контролируемое исследование Moraes Fiho [22], в котором также сравнивали вагинальное введение 25 мкг мизопростола каждые 6 ч и родовозбуждение путем интрацервикального введения катетера Фолея с последующей инфузией окситоцина. Средний интервал «родовозбуждение — роды» был более коротким при применении простагландина Е1, чем при применении катетера Фолея и окситоцина (17 и 20 ч соответственно). Различий по аномалиям родовой деятельности, частоте кесарева сечения выявлено не было. Таким образом, применение мизопростола для родовозбуждения было эффективным и безопасным.
Внимания также заслуживают исследования, опубликованные в 2015 г. В одном из них [23] сравнивали вагинальное введение мизопростола и применение катетера Фолея в комбинации с интравагинальным применением изосорбида мононитрата. Исследование было рандомизированным, включало 395 пациенток. Основным показателем неэффективности родовозбуждения была частота последующего кесарева сечения. Авторами с большой достоверностью было показано, что при применении мизопростола частота оперативного родоразрешения была ниже, чем при использовании баллонного расширения шейки матки и изосорбида мононитрата (22,8 и 33,3 %) (р < 0,001). Продолжительность родовозбуждения также была меньше в группе, в которой применялся простагландин Е1. В то же время в этой группе гиперстимуляция матки встречалась достоверно чаще. Главным выводом этого исследования стало то, что применение мизопростола было более эффективным, но менее безопасным, чем комбинация катетера Фолея и изосорбида мононитрата.
В исследование Chavakula, Benjamin [24], также опубликованное в 2015 г., вошли 100 женщин с задержкой развития плода. Применялось вагинальное введение 25 мкг мизопростола каждые 6 ч и интрацервикальное введение катетера Фолея. Целью была оценка частоты тахисистолии и появления аномалий сердечного ритма у плода, а также сравнивались эффективность родовозбуждения и наличие осложнений родового акта. Только у одной роженицы из группы, получивших простагландин Е1 зафиксирован эпизод тахисистолии плода. Частота неэффективного родовозбуждения, закончившегося операцией кесарева сечения, была больше в группе, в которой применялся катетер Фолея (26 %). При применении мизопростола роды в течение 12 ч от начала родовозбуждения происходили чаще (26,1 и 5,6 %). Другие осложнения родов были немногочисленными в обеих группах. Вагинальное применение мизопростола для индукции родов у женщин с задержкой развития плода оказалось более эффективным, чем применение катетера Фолея. Кратко результаты описанных исследований представлены в табл. 2.
Таблица 2. Сравнение мизопростола и баллонного расширения шейки матки с целью родовозбуждения
Table 2. Comparison of misoprostol and balloon dilation of the cervix for the purpose of labor induction
Автор | Год | Тип исследования | Сравниваемые методы родовозбуждения | Основные результаты |
Abramovici | 1999 | Клиническое исследование | Мизопростол перорально, катетер Фолея интрацервикально + окситоцин | Интервал от начала индукции до начала схваток у первородящих больше при применении мизопростола, нет различий в перинатальных исходах |
Culver | 2004 | Клиническое исследование | Мизопростол вагинально и катетер Фолея интрацервикально | Интервал от начала индукции до начала схваток больше при применении мизопростола. Нет различий по отсутствию эффекта от родовозбуждения |
Moraes | 2010 | Клиническое исследование | Мизопростол вагинально и катетер фолея интрацервикально + окситоцин | При применении мизопростола интервал от начала индукции до начала схваток меньше, нет различий по частоте кесарева сечения и аномалиям родовой деятельности |
Chavakula | 2015 | Клиническое исследование | Мизопростол вагинально и катетер Фолея интрацервикально | Отсутствие эффекта от родовозбуждения чаще при использовании катетера Фолея, перинатальные исходы не отличались |
El-Khayat | 2015 | Клиническое исследование | Мизопростол вагинально, катетер Фолея интрацервикально + изосорбид мононитрат | Частота кесарева сечения при применении мизопростола ниже, гиперстимуляция матки чаще встречается при применении мизопростола |
Применение мизопростола у женщин с рубцом на матке
Внимания также заслуживает применение мизопростола с целью родовозбуждения у женщин с оперированной маткой. Впервые клинический протокол родовозбуждения у беременных с рубцом на матке был проведен в 1999 г. Wing [25]. Cравнивали применение мизопростола интравагинально и окситоцина у женщин с рубцом на матке после операции кесарева сечения. Описано 2 случая разрыва матки по старому рубцу, повлекшие за собой экстренное кесарево сечение, длительное нахождение пациенток и новорожденных в стационаре. Разрывы матки были бессимптомными и диагностировались во время лапаротомий, предпринятых в связи с дистрессом плода. Однако в исследование также вошли 17 женщин с рубцом на матке после операции кесарева сечения, получивших мизопростол, роды у которых протекали без осложнений, дети родились в удовлетворительном состоянии. Авторы рекомендуют проявлять осторожность в таких случаях.
В метаанализе Sanchez-Ramos et al. в 2000 г. [26] было показано, что разрывы матки встречались в 4,5 % случаев, однако исследования были немногочисленными.
Следует отметить, что проблема применения мизопростола у женщин с оперированной маткой продолжает изучаться. Последнее ретроспективное когортное исследование было опубликовано в 2016 г. [27]. Изучалась частота разрывов матки у 208 женщин с одним рубцом на матке после операции кесарева сечения, которые были разделены на две группы в зависимости от метода индукции родов. В первую группу были включены пациентки, которым было применено родовозбуждение динопростоном, окситоцином и механическими методами, а во вторую — пациентки, которым применено родовозбуждение пероральным введением мизопростола. Показано, что разрывы матки встречались в 4,3 % случаев в обеих группах. Не было получено статистических различий по частоте возникновения разрывов матки в зависимости от метода родовозбуждения. Авторами сделан вывод о том, что оральное применение мизопростола у женщин с рубцом на матке не увеличивает частоту разрывов матки.
Таким образом, несмотря на большое количество выполненных исследований, их данные противоречивы. В исследованиях применялся разный дизайн, схемы родовозбуждения не были одинаковыми, не всегда количество пациенток было достаточным. Кроме того, до настоящего времени не определена оптимальная методика родовозбуждения. Каждый метод обладает как преимуществами, так и недостатками. Нет единого мнения о целесообразной дозе, способе и интервале введения мизопростола. Не разработан «золотой стандарт» индукции родов. По мнению большинства авторов, требуются дальнейшие исследования с более четким дизайном и большим количеством пациенток. Необходима разработка алгоритма методов родовозбуждения с применением простагландина Е1.
About the authors
Gleb V Blagodarniy
FSBSI “The Research Institute of Obstetrics, Gynecology and Reproductology named after D.O. Ott”
Author for correspondence.
Email: glebblag@mail.ru
graduate student, dep. labor and delivery Russian Federation
References
- Баскетт Т.Ф., Калдер Э.А. Оперативное акушерство Манро Керра. – М.: Логосфера, 2015. [Baskett TF, Kalder JeA. Operativnoe akusherstvo Manro Kerra. Moscow: Logosfera; 2015. (In Russ.)]
- WHO recommendations for Induction of labour. Available at: http://www.who.int/reproductivehealth/publications/maternal_perinatal_health/9789241501156/ru/.
- Северин Е.С., ред. Биохимия: учеб. для вузов. – М., 2003. [Severin ES, red. Biohimija: ucheb. dlja vuzov. Moscow; 2003. (In Russ.)]
- Сидельникова В.М. Эндокринология беременности в норме и при патологии. – М.: Медпресс, 2009. [Sidel’nikova VM. Jendokrinologija beremennosti v norme i pri patologii. Moscow: Medpress; 2009. (In Russ.)]
- Arulkumaran S, Kandola MK, Hoffman BJ, et al. The roles of prostaglandin EP1 and 3 receptors in the control of human myometrial contractility. Clin Endocrinol Metab. 2012;97(2):489-98. doi: 10.1210/jc.2011-1991.
- Zieman M, Fong SK, Benowitz NL, et al. Absorption kinetics of misoprostol with oral or vaginal administration. Obstet Gynecol. 1997;90(1):88-92.
- Tang OS, Gemzell-Danielsson K, Ho PC. Misoprostol: pharmacokinetic profiles, effects on the uterus and side-effects. Int J Gynecology Obstet. 2007;99:S160-7.
- Hofmeyr GJ, Gülmezoglu AM, Alfirevic Z. Misoprostol for induction of labour: a systematic review. Br J Obstet Gynaecol. 1999;106(8):798-803.
- Wing DA, Ham D, Paul RH. A comparison of orally administered misoprostol with vaginally administered misoprostol for cervical ripening and labor induction. Am J Obstet Gynecol. 1999;180(5):1155-60.
- Kundodyiwa TW, Alfirevic Z, Weeks AD. Low-dose oral misoprostol for induction of labor: a systematic review. Obstet Gynecol. 2009;113(2 Pt 1):374-83. doi: 10.1097/AOG.0b013e3181945859.
- Deshmukh VL, Yelikar KA, Waso V. Comparative study of efficacy and safety of oral versus vaginal misoprostol for induction or labour. J Obstet Gynaecol India. 2013;63(5):321-4. doi: 10.1007/s13224-012-0337-3.
- Komala K, Reddy M, Quadri IJ. Comparative study of oral and vaginal misoprostol for induction of labour, maternal and foetal outcome. J Clin Diagn Res. 2013;7(12): 2866-9. doi: 10.7860/JCDR/2013/5825.3779.
- Alfirevic Z, Keeney E, Dowswell T, et al. Labour induction with prostaglandins: a systematic review and network meta analysis. BMJ. 2015;350: h217. doi: 10.1136/bmj.h217.
- Cheng SY, Hsue CS, Hwang GH, et al. Comparison of labor induction with titrated oral misoprostol solution between nulliparous and multiparous women. J Obstet Gynaecol Res. 2010;36(1):72-8. doi: 10.1111/j.1447-0756.2009.01118.x.
- Cheng SY, Ming H, Lee JC. Titrated oral compared with vaginal misoprostol for labor induction: a randomized controlled trial. Obstet Gynecol. 2008;111(1):119-25. doi: 10.1097/01.AOG.0000297313.68644.71.
- Souza AS, Feitosa FE, Costa AA, et al. Titrated oral misoprostol solution versus vaginal isoprostol for labor induction. Int J Gynaecol Obstet. 2013;123(3):207-12. doi: 10.1016/j.ijgo.2013.06.028.
- Crane JM, Butler B, Young DC, Hannah ME. Misoprostol compared with prostaglandin E2 for labour induction in women at term with intact membranes and unfavourable cervix: a systematic review. BJOG. 2006;113(12):1366-76.
- Ozkan S, Calişkan E, Doğer E, et al. Comparative efficacy and safety of vaginal misoprostol versus dinoprostone vaginal insert in labor induction at term: a randomized trial. Arch Gynecol Obstet. 2009;280(1):19-24. doi: 10.1007/s00404-008-0843-9.
- Petersen JF, Bergholt T, Løkkegaard EC. Safe induction of labour with low-dose misoprostol, but less effective than the conventional dinoprostone regimen. Dan Med J. 2013;60(9): A4706.
- Abramovici D, Goldwasser S, Mabie BC, et al. A randomized comparison of oral misoprostol versus Foley catheter and oxytocin for induction of labor at term. Am J Obstet Gynecol. 1999;181(5 Pt 1):1108-12.
- Culver J, Strauss RA, Brody S, et al. A randomized trial comparing vaginal misoprostol versus Foley catheter with concurrent oxytocin for labor induction in nulliparous women. Am J Perinatol. 2004;21(3):139-46.
- Moraes Filho OB, Albuquerque RM, Cecatti JG. A randomized controlled trial comparing vaginal misoprostol versus Foley catheter plus oxytocin for labor induction. Acta Obstet Gynecol Scand. 2010;89(8):1045-52. doi: 10.3109/00016349.2010.499447.
- El-Khayat W, Alelaiw H, El-kateb A, Elsemary A. Comparing vaginal misoprostol versus Foley catheter plus vaginal isosorbide mononitrate for labor induction. J Matern Fetal Neonatal Med. 2016;29(3):487-92. doi: 10.3109/14767058.2015.1007036.
- Chavakula PR, Benjamin SJ, Abraham A, et al. Misoprostol versus Foley catheter insertion for induction of labor in pregnancies affected by fetal growth restriction. Int J Gynaecol Obstet. 2015;129(2):152-5. doi: 10.1016/j.ijgo.2014.11.018.
- Wing DA, Lovett K, Paul RH. Disruption of prior uterine incision following misoprostol for labor induction in women with previous cesarean delivery. Obstet Gynecol. 1998;91(5 Pt 2):828-30.
- Sanchez-Ramos L, Kaunitz AM. Misoprostol for cervical ripening and labor induction: a systematic review of the literature. Clin Obstet Gynecol. 2000;43(3):475-88.
- Stenson D, Wallstrom T, Sjostrand M, et al. Induction of labor in women with a uterine scar. J Matern Fetal Neonatal Med. 2016;29(20):3286-91. doi: 10.3109/14767058.2015.1123242.
Supplementary files








